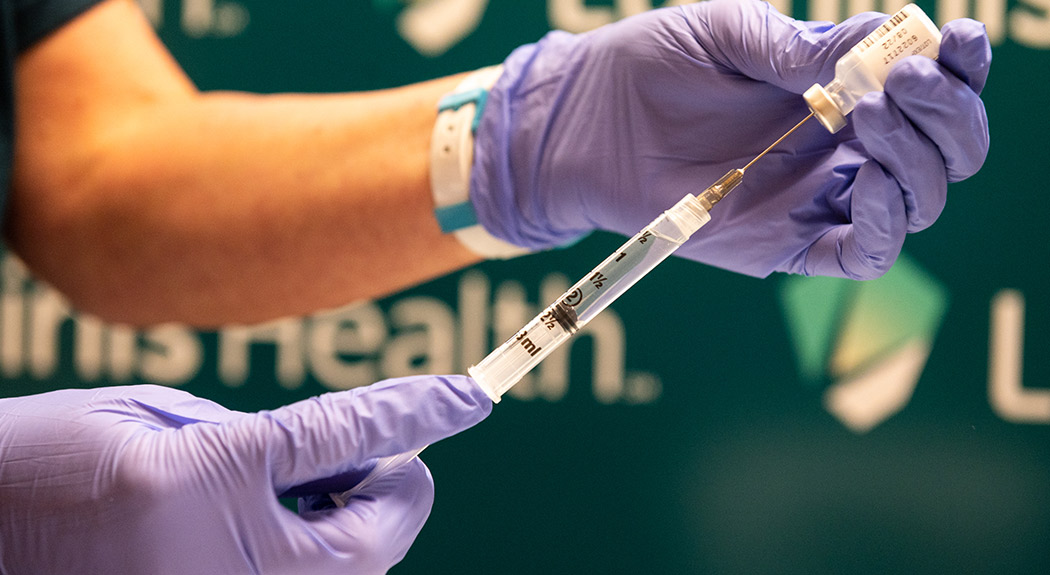
You can’t turn on the news or scroll through social media today without hearing about the COVID-19 vaccine. And while we know you’re anxious to put the pandemic behind you, we also know you may have lingering questions about the vaccine.
You aren’t alone. Many of your coworkers, family members and neighbors are wrestling with the same questions. We’ve never experienced a pandemic of this magnitude in our lifetimes, and we’ve never seen a vaccine developed this quickly. But investigating the details and unpacking what we know about the vaccine can go a long way in helping you feel more at ease.
It’s important to know that multiple COVID-19 vaccines are under development. At this time, Pfizer and Moderna are the only vaccines available in the United States. They are the only COVID-19 vaccines that have received an Emergency Use Authorization (EUA) from the Food and Drug Administration (FDA).
Fast doesn’t mean careless.
It’s true; this vaccine is one of the fastest developed in modern history. But researchers were not starting from scratch when they learned about SARS-CoV-2, the virus that causes COVID-19.
Both the Pfizer and Moderna vaccines are messenger RNA (mRNA) vaccines. Technology associated with the mRNA vaccine dates back to the 1990s. According to the Centers for Disease Control (CDC), researchers performed early stage clinical trials using mRNA vaccines for HIV, influenza, Zika, rabies, and others.
Unfortunately, it has taken a pandemic to get the needed funding to push this technology forward to develop this type of vaccine.
It’s also important to note the process has been able to move so quickly because:
- The clinical trials were centrally coordinated by the government rather than various pharmaceutical agencies.
- The clinical trials combined the first two phases to assess safety, dosing, and the immune responses.
- The FDA granted the Pfizer and Moderna vaccines an EUA to allow for quick approval and distribution. Under an EUA, approval is pushed ahead of less critical projects. In order to issue an EUA, FDA must determine the known and potential benefits of the vaccine outweigh its known and potential risks. CDC continues assessing the effectiveness of vaccines approved for an EUA.
None of the factors that allowed the accelerated development of a COVID-19 vaccine have compromised safety, scientific or ethical integrity. No short-cuts have been made.
The FDA recommends a vaccine have an effectiveness rate of at least 50 percent. Both the Pfizer and Moderna vaccines far exceed this standard. Both report about 95 percent effectiveness at preventing symptoms of COVID-19, including severe disease. This efficacy rate is extraordinary.
You won’t get COVID from the vaccine, but you may experience mild flu-like symptoms.
It’s not possible to get COVID-19 from the vaccine. Pfizer and Moderna vaccines only produce the spike protein from the virus, not the whole virus.
However, when you get the vaccine you may experience some side effects, including chills, fatigue, headache, joint and muscle pain and injection site pain. But these side effects are typically mild and will go away on their own within one or two days. They represent immune activation and are seen with other vaccinations.
It takes a few weeks for the body to build immunity after vaccination. That means it’s possible you could be infected with the virus that causes COVID-19 just before or just after vaccination and get sick. It takes about two weeks after your second dose for full immunity.
Two doses of the vaccine are necessary.
Both the Pfizer and Moderna vaccines require two doses to be effective. Pfizer’s second shot occurs three weeks after the first dose, and Moderna’s is four weeks. Health experts recommend you resist the urge to skip the second dose and make time for the second shot.
Vaccines for all will take several months.
Vaccine distribution will take a while to make it into your neighborhood. That’s because the Maryland Department of Health created a phased approach to vaccine distribution based on initial limited supplies. First available doses will go to those at highest risk of exposure to or developing complications from COVID-19, including hospital health care workers and nursing home residents and staff. Next up will be first responders and those at significant risk of severe COVID-19 symptoms. Phase 2 targets essential non-health care and transportation workers, and people at moderately higher risk of severe COVID-19 illness. Phase 3 focuses on vaccinations for the general public.
According to the CDC, vaccines should be available to the general public by the spring of 2021 and distributed throughout the year.
Now is not the time to let your guard down.
Just because a vaccine is making its way into your area, it still isn’t time to let your guard down. It will take a while for everyone to get both doses of the vaccine. For a highly contagious disease like COVID-19, much of the population must be vaccinated to achieve herd immunity. Herd immunity occurs when enough people become immune to COVID-19 to make its spread unlikely.
And, while Pfizer and Moderna vaccines show they’re about 95 percent effective at protecting you from the disease, they aren’t 100 percent effective. That means there’s a small chance you can still get COVID-19 after being vaccinated if you’re exposed.
Experts recommend continuing all of the safety measures we know are working to keep the virus at bay, including the 3Ws: Wash your hands. Wear a mask. Watch your distance.
For your health and safety, stay up to date.
Information about the pandemic and the vaccine changes daily. For the latest recommendations for you and your family, listen to your local public health officials and bookmark the CDC’s vaccination page for the most up to date information.